 As Florida — and indeed our nation — begins to contemplate how we can “reopen for business,” the health care community is asking the same questions. How can we do this safely? What’s necessary? What is not?
As Florida — and indeed our nation — begins to contemplate how we can “reopen for business,” the health care community is asking the same questions. How can we do this safely? What’s necessary? What is not?
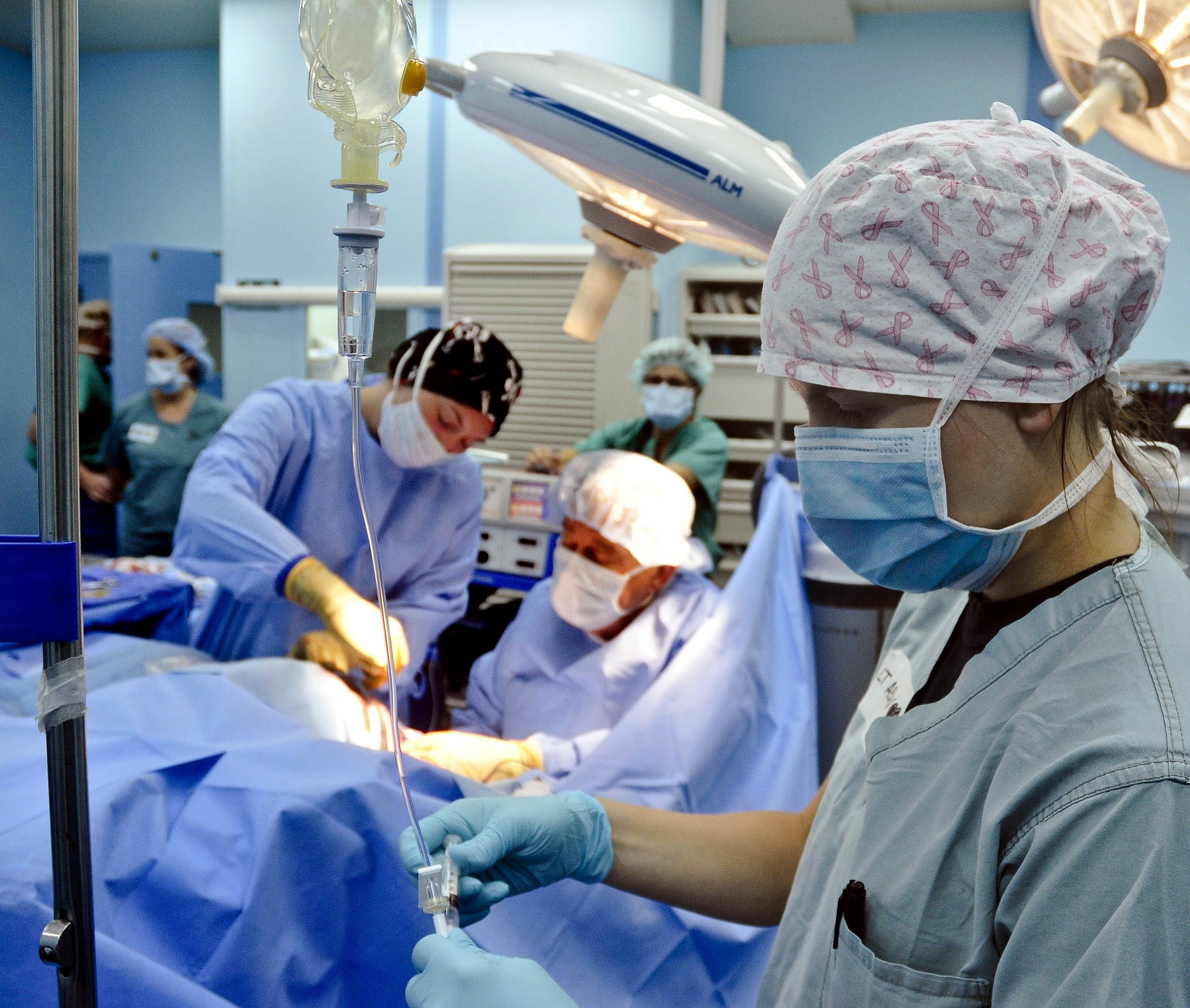
Physician anesthesiologists, as leaders in perioperative medicine, can offer expert counsel on getting our medical community back online.
As a patient safety and advocacy organization, the Florida Society of Anesthesiologists (FSA) in March joined other groups advising a cautious approach that limited most procedures as the health care system braced for the COVID crisis.
During the emergency, in order to ensure the adequate capacity of critical care services and accompanying resources, local and state governments followed the wise lead of Gov. Ron DeSantis and smartly suspended all nonemergent or “elective” surgeries and procedures.
Florida’s physician anesthesiologists then served in many capacities in taking care of the sickest and most-in-need patients in the state.
Due to extensive years of education and thousands of hours of clinical training, anesthesiology doctors were deployed throughout the state and nation, performing the most dangerous bedside procedures on critically ill COVID-19 patients.
The Governor’s forward-thinking recommendations likely averted a true public health crisis in our state. As the new infection rate has started to level off, the public, patients, hospital systems, and ambulatory surgery centers are left wondering when the time is right to reopen.
The primary reason to resume these surgeries is to help patients who are suffering from a wide variety of painful or chronic medical conditions for whom the operating room or interventional pain clinic provides hope of relief.
Other Floridians may need diagnostic procedures to better determine their course of medical treatment. With that, we must stress the importance of a set of guiding principles that protect patients and front-line health care workers while at the same time responsibly conserving limited medical resources.
The FSA and other like-minded patient-centric organizations can offer guidance for public officials and health care leaders as reopening agendas are contemplated.
The “Readiness Roadmap,” a joint statement released by the American Society of Anesthesiologists, the American College of Surgeons, the Association of periOperative Registered Nurses and the American Hospital Association addresses many of the issues relevant to the resumption of nonemergent, but pressingly necessary, procedures.
As we transition the medical delivery systems back to “normal,” it is important to understand that nonemergent surgeries are much more than “elective” cases such as “tummy tucks” or other cosmetic procedures.
Examples of “elective” procedures that were delayed, much to the rightful concern of affected patients, include the repair of torn knee ligaments, back surgery to fix a damaged disk, heart stent insertions, injections to relieve acute or chronic pain, and the removal of cancerous or precancerous lesions.
In fact, most “elective” surgeries are medically necessary but are not immediately required.
The leadership and experience of anesthesiologists should give confidence to patients, other physicians, health care workers, and industry executives when it is safe to proceed in a measured manner with elective surgeries and procedures.
As we evaluate the geographic density of COVID cases among the “worried well,” the availability of appropriate protective medical resources, and the triage of necessary cases, we urge a go-forward-cautiously approach always guided by the primacy of patient safety first.
___
Dr. Jay Epstein received his medical degree at Case Western Reserve University before doing his anesthesiology residency and critical care medicine fellowship at the Johns Hopkins Hospital. He is board-certified in both specialties and works in private practice as a partner at Greater Florida Anesthesiologists, a division of Envision Healthcare.



